Abstract
Background
We compared outcomes of surgery and radiofrequency thermal ablation (RFA) in patients with metachronous liver metastases.
Methods
Between October 1995 and December 2005, 59 patients underwent hepatic resection and 30 underwent RFA for metachronous liver metastases. Patients with extra-hepatic metastases, those who underwent both types of treatment, and those with synchronous hepatic metastasis were excluded.
Results
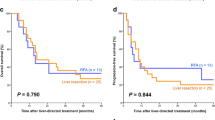
The two groups had similar mean age, sex ratio, comorbid medical conditions, primary disease stage, and frequency of solitary metastases. Preoperative mean serum carcinoembryonic antigen (CEA) level was significantly higher in the RFA group (13.4 ng/mL vs. 7.7 ng/mL; p = 0.02). Mean diameter of hepatic metastases was significantly greater in the resection than in the RFA group (3.1 cm vs. 2.0 cm; p = 0.001). Recurrence after treatment of metastasis was observed in 18 of 30 (60.0%) RFA and 33 of 59 (56%) resection patients. Local recurrence at the RFA site was observed in 7 of 30 (23%) patients. Time to recurrence (15 vs. 8 months, p = 0.02) and overall survival (56 vs. 36 months, p = 0.005) were significantly longer in the resection than in the RFA group. In the 69 patients with solitary metastases of diameter ≤3 cm, time to recurrence (p = 0.004) and overall survival were significantly greater in the resection group.
Conclusions
Compared with hepatic resection, RFA for metachronous hepatic metastases from colorectal cancer was associated with higher local recurrence and shorter recurrence-free and overall survival rates, even in patients with solitary, small (≤3 cm) lesions.

Similar content being viewed by others
References
Scheele J, Stang R, Altendorf-Hofmann A, Paul M. Resection of colorectal liver metastases. World J Surg 1995;19:59–71
Rees M, Plant G, Bygrave S. Late results justify resection for multiple hepatic metastases from colorectal cancer. Br J Surg 1997;84:1136–1140
Steele G Jr, Bleday R, Mayer RJ, Lindblad A, Petrelli N, Weaver D. A prospective evaluation of hepatic resection for colorectal carcinoma metastases to the liver: Gastrointestinal Tumor Study Group Protocol 6584. J Clin Oncol 1991;9:1105–1112
Fong Y, Fortner J, Sun RL, Brennan MF, Blumgart LH. Clinical score for predicting recurrence after hepatic resection for metastatic colorectal cancer: analysis of 1001 consecutive cases. Ann Surg 1999;230:309–318
Nordlinger B, Guiguet M, Vaillant JC, Balladur P, Boudjema K, Bachellier P, et al. Surgical resection of colorectal carcinoma metastases to the liver. A prognostic scoring system to improve case selection, based on 1568 patients. Association Francaise de Chirurgie. Cancer 1996;77:1254–1262
Choti MA, Sitzmann JV, Tiburi ME, Sumetchotimetha W, Rangsin R, Schulick RD, et al. Trends in long-term survival following liver resection for hepatic colorectal metastases. Ann Surg 2002;235:759–766
Abdalla EK, Vauthey JN, Ellis LM, Ellis V, Pollock R, Broglio KR, et al. Recurrence and outcomes following hepatic resection, radiofrequency ablation, and combined resection/ablation for colorectal liver metastases. Ann Surg 2004; 239:818–825
Pawlik TM, Scoggins CR, Zorzi D, Abdalla EK, Andres A, Eng C, et al. Effect of surgical margin status on survival and site of recurrence after hepatic resection for colorectal metastases. Ann Surg 2005;241:715–722
Cady B, Stone MD. The role of surgical resection of liver metastases in colorectal carcinoma. Semin Oncol 1991;18:399–406
Livraghi T, Solbiati L, Meloni F, Ierace T, Goldberg SN, Gazelle GS. Percutaneous radiofrequency ablation of liver metastases in potential candidates for resection: the “test-of-time approach”. Cancer 2003;97:3027–3035
Solbiati L, Livraghi T, Goldberg SN, Ierace T, Meloni F, Dellanoce M, et al. Percutaneous radio-frequency ablation of hepatic metastases from colorectal cancer: long-term results in 117 patients. Radiology 2001;221:159–166
Lencioni R, Goletti O, Armillotta N, Paolicchi A, Moretti M, Cioni D, et al. Radio-frequency thermal ablation of liver metastases with a cooled-tip electrode needles: results of a pilot clinical trial. Eur Radiol 1998;8:1205–1211
Elias D, Baton O, Sideris L, Matsuhisa T, Pocard M, Lasser P. Local recurrence after intraoperative radiofrequency ablation of liver metastases: a comparative study with anatomic and wedge resections. Ann Surg Oncol 2004;11:500–505
Oshowo A, Gillams A, Harrison E, Lees WR, Taylor I. Comparison of resection and radiofrequency ablation for treatment of solitary colorectal liver metastases. Br J Surg 2003;90:1240–1243
Solbiati L, Ierace T, Goldberg SN, Sironi S, Livraghi T, Fiocca R, et al. Percutaneous US-guided radiofrequency ablation of liver metastases: treatment and follow-up in 16 patients. Radiology 1997;202:195–203
Lencioni R, Crocetti L, Cioni D, Della Pina C, Bartolozzi C. Percutaneous radiofrequency ablation of hepatic colorectal metastases: technique, indications, results, and new promises. Invest Radiol 2004;39:689–697
Aloia TA, Vauthey JN, Loyer EM, Ribero D, Pawlik TM, Wei SH, et al. Solitary colorectal liver metastasis: resection determines outcome. Arch Surg 2006;141:460–467
Wagner JS, Adson MA, Van Heerden JA, Adson MH, Ilstrup DM. The natural history of hepatic metastases form colorectal cancer. A comparison with resective treatment. Ann Surg 1984;199:502–508
Scheele J, Stangl R, Attendorf-Hofmann A, Gall FP. Indicatiors of prognosis after hepatic resection for colorectal secondaries. Surgery 1991;110:13–29
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Park, I.J., Kim, H.C., Yu, C.S. et al. Radiofrequency Ablation for Metachronous Liver Metastasis from Colorectal Cancer after Curative Surgery. Ann Surg Oncol 15, 227–232 (2008). https://doi.org/10.1245/s10434-007-9625-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-007-9625-z