Abstract
Purpose
To clarify the need for post-operative radiation treatment in skull base chondrosarcomas (SBCs).
Methods
A retrospective analysis of patients with grade I or II SBC. Patients were divided according to post-surgical treatment strategies: (A) planned upfront radiotherapy and (B) watchful waiting. Tumor control and survival were compared between the treatment groups. The median follow-up after resection was 105 months (range, 9–376).
Results
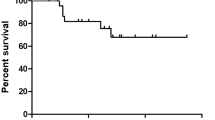
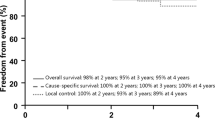
Thirty-two patients (Grade 1, n = 16; Grade 2, n = 16) were included. The most frequent location was petroclival (21, 64%). A gross total resection (GTR) was achieved in 11 patients (34%). Fourteen (44%) underwent upfront radiotherapy (group A) whereas 18 (56%) were followed with serial MRI alone (group B). The tumor control rate for the entire group was 77% and 69% at 10- and 15-year, respectively. Upfront radiotherapy (P = 0.25), extent of resection (P = 0.11) or tumor grade (P = 0.83) did not affect tumor control. The majority of Group B patients with recurrent tumors (5/7) obtained tumor control with repeat resection (n = 2), salvage radiotherapy (n = 2), or a combination of both (n = 1). The 10-year disease-specific survival was 95% with no difference between the group A and B (P = 0.50).
Conclusion
For patients with grade I/II SBC, a reasonable strategy is deferral of radiotherapy after maximum safe resection until tumor progression or recurrence. At that time, most patients can be successfully managed with salvage radiotherapy or surgery. Late recurrences may occur, and life-long follow-up is advisable.


Similar content being viewed by others
Data Availability
The data will be available upon reasonable request to the corresponding author.
References
Evans HL, Ayala AG, Romsdahl MM (1977) Prognostic factors in chondrosarcoma of bone: a clinicopathologic analysis with emphasis on histologic grading. Cancer 40(2):818–831
Weber AL, Brown EW, Hug EB, Liebsch NJ (1995) Cartilaginous tumors and chordomas of the cranial base. Otolaryngol Clin North Am 28(3):453–471
Awad M, Gogos AJ, Kaye AH (2016) Skull base chondrosarcoma. J Clin Neurosci 24:1–5. https://doi.org/10.1016/j.jocn.2015.10.029
Bloch OG, Jian BJ, Yang I, Han SJ, Aranda D, Ahn BJ, Parsa AT (2009) A systematic review of intracranial chondrosarcoma and survival. J Clin Neurosci 16(12):1547–1551. https://doi.org/10.1016/j.jocn.2009.05.003
Mokhtari S, Mirafsharieh A (2012) Clear cell chondrosarcoma of the head and neck. Head Neck Oncol 4:13. https://doi.org/10.1186/1758-3284-4-13
Nakashima Y, Unni KK, Shives TC, Swee RG, Dahlin DC (1986) Mesenchymal chondrosarcoma of bone and soft tissue. A review of 111 cases. Cancer 57(12):2444–2453
Ma XJ, Meng GL, Wang K, Li D, Wang L, Li H, Zhang JT, Zhang LW, Wu Z (2019) The differences between intracranial mesenchymal chondrosarcoma and conventional chondrosarcoma in clinical features and outcomes. World Neurosurg 122:E1078–E1082. https://doi.org/10.1016/j.wneu.2018.10.230
Amer KM, Munn M, Congiusta D, Abraham JA, Basu Mallick A (2020) Survival and prognosis of chondrosarcoma subtypes: SEER database analysis. J Orthop Res 38(2):311–319. https://doi.org/10.1002/jor.24463
Korten AG, ter Berg HJ, Spincemaille GH, van der Laan RT, Van de Wel AM (1998) Intracranial chondrosarcoma: review of the literature and report of 15 cases. J Neurol Neurosurg Psychiatry 65(1):88–92
Carlson ML, O’Connell BP, Breen JT, Wick CC, Driscoll CL, Haynes DS, Thompson RC, Isaacson B, Gidley PW, Kutz JW Jr, Van Gompel JJ, Wanna GB, Raza SM, DeMonte F, Barnett SL, Link MJ (2016) Petroclival chondrosarcoma: A multicenter review of 55 cases and new staging system. Otol Neurotol 37(7):940–950. https://doi.org/10.1097/MAO.0000000000001037
Gatfield ER, Noble DJ, Barnett GC, Early NY, Hoole ACF, Kirkby NF, Jefferies SJ, Burnet NG (2018) Tumour volume and dose influence outcome after surgery and high-dose photon radiotherapy for chordoma and chondrosarcoma of the skull base and spine. Clin Oncol (R Coll Radiol) 30(4):243–253. https://doi.org/10.1016/j.clon.2018.01.002
Simon F, Feuvret L, Bresson D, Guichard JP, El Zein S, Bernat AL, Labidi M, Calugaru V, Froelich S, Herman P, Verillaud B (2018) Surgery and protontherapy in Grade I and II skull base chondrosarcoma: A comparative retrospective study. PLoS ONE 13(12):e0208786. https://doi.org/10.1371/journal.pone.0208786
Weber DC, Badiyan S, Malyapa R, Albertini F, Bolsi A, Lomax AJ, Schneider R (2016) Long-term outcomes and prognostic factors of skull-base chondrosarcoma patients treated with pencil-beam scanning proton therapy at the Paul Scherrer Institute. Neuro Oncol 18(2):236–243. https://doi.org/10.1093/neuonc/nov154
Holtzman AL, Rotondo RL, Rutenberg MS, Indelicato DJ, Mercado CE, Rao D, Tavanaiepour D, Morris CG, Louis D, Flampouri S, Mendenhall WM (2019) Proton therapy for skull-base chondrosarcoma, a single-institution outcomes study. J Neurooncol 142(3):557–563. https://doi.org/10.1007/s11060-019-03129-8
Koga T, Shin M, Saito N (2010) Treatment with high marginal dose is mandatory to achieve long-term control of skull base chordomas and chondrosarcomas by means of stereotactic radiosurgery. J Neurooncol 98(2):233–238. https://doi.org/10.1007/s11060-010-0184-y
Uhl M, Mattke M, Welzel T, Oelmann J, Habl G, Jensen AD, Ellerbrock M, Haberer T, Herfarth KK, Debus J (2014) High control rate in patients with chondrosarcoma of the skull base after carbon ion therapy: first report of long-term results. Cancer 120(10):1579–1585. https://doi.org/10.1002/cncr.28606
Amichetti M, Amelio D, Cianchetti M, Enrici RM, Minniti G (2010) A systematic review of proton therapy in the treatment of chondrosarcoma of the skull base. Neurosurg Rev 33(2):155–165. https://doi.org/10.1007/s10143-009-0234-0
Sahgal A, Chan MW, Atenafu EG, Masson-Cote L, Bahl G, Yu E, Millar BA, Chung C, Catton C, O’Sullivan B, Irish JC, Gilbert R, Zadeh G, Cusimano M, Gentili F, Laperriere NJ (2015) Image-guided, intensity-modulated radiation therapy (IG-IMRT) for skull base chordoma and chondrosarcoma: preliminary outcomes. Neuro Oncol 17(6):889–894. https://doi.org/10.1093/neuonc/nou347
Mattke M, Vogt K, Bougatf N, Welzel T, Oelmann-Avendano J, Hauswald H, Jensen A, Ellerbrock M, Jakel O, Haberer T, Herfarth K, Debus J, Uhl M (2018) High control rates of proton- and carbon-ion-beam treatment with intensity-modulated active raster scanning in 101 patients with skull base chondrosarcoma at the Heidelberg Ion Beam Therapy Center. Cancer 124(9):2036–2044. https://doi.org/10.1002/cncr.31298
Li D, Weng JC, Zhang GJ, Hao SY, Tang J, Zhang LW, Wang L, Wu Z, Jia W, Zhang JT (2018) Proposed treatment paradigm for intracranial chondrosarcomas based on multidisciplinary coordination. World Neurosurg 109:e517–e530. https://doi.org/10.1016/j.wneu.2017.10.013
Raza SM, Gidley PW, Meis JM, Grosshans DR, Bell D, DeMonte F (2017) Multimodality treatment of skull base chondrosarcomas: the role of histology specific treatment protocols. Neurosurgery 81(3):520–530. https://doi.org/10.1093/neuros/nyx042
Tzortzidis F, Elahi F, Wright DC, Temkin N, Natarajan SK, Sekhar LN (2006) Patient outcome at long-term follow-up after aggressive microsurgical resection of cranial base chondrosarcomas. Neurosurgery 58(6):1090–1098; discussion 1090–1098. https://doi.org/10.1227/01.NEU.0000215892.65663.54
Sbaihat A, Bacciu A, Pasanisi E, Sanna M (2013) Skull base chondrosarcomas: surgical treatment and results. Ann Otol Rhinol Laryngol 122(12):763–770
Vaz-Guimaraes F, Fernandez-Miranda JC, Koutourousiou M, Hamilton RL, Wang EW, Snyderman CH, Gardner PA (2017) Endoscopic endonasal surgery for cranial base chondrosarcomas. Oper Neurosurg (Hagerstown) 13(4):421–434. https://doi.org/10.1093/ons/opx020
Hasegawa H, Shin M, Kondo K, Hanakita S, Mukasa A, Kin T, Saito N (2018) Role of endoscopic transnasal surgery for skull base chondrosarcoma: a retrospective analysis of 19 cases at a single institution. J Neurosurg 128(5):1438–1447. https://doi.org/10.3171/2017.1.JNS162000
Samii A, Gerganov V, Herold C, Gharabaghi A, Hayashi N, Samii M (2009) Surgical treatment of skull base chondrosarcomas. Neurosurg Rev 32(1):67–75; discussion 75. https://doi.org/10.1007/s10143-008-0170-4
Cho YH, Kim JH, Khang SK, Lee JK, Kim CJ (2008) Chordomas and chondrosarcomas of the skull base: comparative analysis of clinical results in 30 patients. Neurosurg Rev 31(1):35–43; discussion 43. https://doi.org/10.1007/s10143-007-0099-z
Almefty K, Pravdenkova S, Colli BO, Al-Mefty O, Gokden M (2007) Chordoma and chondrosarcoma: similar, but quite different, skull base tumors. Cancer 110(11):2457–2467. https://doi.org/10.1002/cncr.23073
Wanebo JE, Bristol RE, Porter RR, Coons SW, Spetzler RF (2006) Management of cranial base chondrosarcomas. Neurosurgery 58(2):249–255; discussion 249–255. https://doi.org/10.1227/01.NEU.0000194834.74873.FB
Oghalai JS, Buxbaum JL, Jackler RK, McDermott MW (2005) Skull base chondrosarcoma originating from the petroclival junction. Otol Neurotol 26(5):1052–1060. https://doi.org/10.1097/01.mao.0000185076.65822.f7
Crockard HA, Cheeseman A, Steel T, Revesz T, Holton JL, Plowman N, Singh A, Crossman J (2001) A multidisciplinary team approach to skull base chondrosarcomas. J Neurosurg 95(2):184–189. https://doi.org/10.3171/jns.2001.95.2.0184
Frezza AM, Cesari M, Baumhoer D, Biau D, Bielack S, Campanacci DA, Casanova J, Esler C, Ferrari S, Funovics PT, Gerrand C, Grimer R, Gronchi A, Haffner N, Hecker-Nolting S, Holler S, Jeys L, Jutte P, Leithner A, San-Julian M, Thorkildsen J, Vincenzi B, Windhager R, Whelan J (2015) Mesenchymal chondrosarcoma: prognostic factors and outcome in 113 patients. A European Musculoskeletal Oncology Society study. Eur J Cancer 51(3):374–381. https://doi.org/10.1016/j.ejca.2014.11.007
Strotman PK, Reif TJ, Kliethermes SA, Sandhu JK, Nystrom LM (2017) Dedifferentiated chondrosarcoma: a survival analysis of 159 cases from the SEER database (2001–2011). J Surg Oncol 116(2):252–257. https://doi.org/10.1002/jso.24650
Lu VM, O’Connor KP, Mahajan A, Carlson ML, Van Gompel JJ (2020) Carbon ion radiotherapy for skull base chordomas and chondrosarcomas: a systematic review and meta-analysis of local control, survival, and toxicity outcomes. J Neurooncol 147(3):503–513. https://doi.org/10.1007/s11060-020-03464-1
Nie Z, Lu Q, Peng H (2018) Prognostic factors for patients with chondrosarcoma: A survival analysis based on the surveillance, epidemiology, and end results (SEER) database (1973–2012). J Bone Oncol 13:55–61. https://doi.org/10.1016/j.jbo.2018.09.003
Funding
None.
Author information
Authors and Affiliations
Contributions
HH: conceptualization, data acquisition, analysis, interpretation, drafting manuscript, final approval of the version to be published. KV: data acquisition, final approval of the version to be published. CSG: conceptualization, data analysis, critically revising manuscript, final approval of the version to be published. MLC: critically revising manuscript, final approval of the version to be published. BEP: interpretation, critically revising manuscript, final approval of the version to be published. PDB: interpretation, critically revising manuscript, final approval of the version to be published. AP: conceptualization, data acquisition, final approval of the version to be published. JJVG: critically revising manuscript, final approval of the version to be published. CLWD: critically revising manuscript, final approval of the version to be published. MJL: conceptualization, interpretation, critically revising manuscript, final approval of the version to be published.
Corresponding author
Ethics declarations
Conflict of interest
The authors have nothing to declare.
Ethical approval
The study was approved by Institutional Review board (IRB #20-002,412).
Consent to participate
Informed consent was waived given the retrospective non-invasive nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hasegawa, H., Vakharia, K., Graffeo, C.S. et al. Long-term outcomes of grade I/II skull base chondrosarcoma: an insight into the role of surgery and upfront radiotherapy. J Neurooncol 153, 273–281 (2021). https://doi.org/10.1007/s11060-021-03764-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-021-03764-0