Abstract
Background
Laparoscopy-assisted distal gastrectomy (LADG) is gaining wider acceptance for the treatment of early gastric cancer. However, firm evidence supporting its safety and usefulness is scant, and no study has compared the outcomes of various procedures for LADG. We examined the surgical outcomes of LADG performed using different methods for lymph node dissection.
Methods
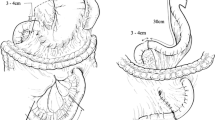
Between September 1998 and January 2005, we performed LADG in 111 patients with early gastric cancer. In the 55 patients treated initially, group 2 lymph node dissection was performed through a small, 7-cm-long incision (minilaparotomy). In 43 of these patients, hand-assisted laparoscopic surgery (HALS) was done. In the 56 patients treated more recently, lymph node dissection was performed laparoscopically. In 31 of these patients, the celiac branches of the vagus nerve were preserved. Clinical outcomes of these procedures were compared.
Results
In the first 55 patients, HALS significantly shortened the operation time (277 vs 243 min, p < 0.05). In the latter 56 patients, LADG with preservation of the celiac branches of the vagus nerve was associated with a longer operation time (283 vs 228 min, p < 0.01) and higher blood loss (150 vs 92 g, p < 0.05) than with LADG without celiac branch preservation. There were no differences among the various operative procedures in postoperative course, including the length of the postoperative hospital stay or the rate of complications.
Conclusions
LADG is a safe and technically feasible procedure for the treatment of early gastric cancer. Laparoscopic lymph node dissection provided a good visual field and was easier to perform and required less time when the celiac branches of the vagus nerve were not preserved, with no negative effect on outcome.
Similar content being viewed by others
References
Adachi Y, Suematsu T, Shiraishi N, Katsuta T, Morimoto A, Kitano S, Akazawa K (1999) Quality of life after laparoscopy-assisted Billroth I gastrectomy. Ann Surg 229: 49–54
Asao T, Hosouchi Y, Nakabayashi T, Haga N, Mochiki E, Kuwano H (2001) Laparoscopically assisted total or distal gastrectomy with lymph node dissection for early gastric cancer. Br J Surg 88: 128–132
Gotoda T, Yanagisawa A, Sasako M, Ono H, Nakanishi Y, Shimoda T, Kato Y (2000) Incidence of lymph node metastasis from early gastric cancer: estimation with a large number of cases at two large centers. Gastric Cancer 3: 219–225
HALS Study Group (2000) Hand-assisted laparoscopic surgery (HALS) with the Hand Port System: initial experience with 68 patients. Ann Surg 231: 715–723
Japan Society for Endoscopic Surgery (2004) Seventh nationwide survey of endoscopic surgery in Japan. Jpn Soc Endosc Surg 9: 495–500
Japanese Gastric Cancer Association (1998) Japanese classification of gastric carcinoma, 2nd English ed. Gastric Cancer 1: 10–24
Japanese Gastric Cancer Association (2001) Guideline for the treatment of gastric cancer. Kanehara-Shuppan, Tokyo, Japan
Kanaya S, Gomi S, Momoi H, Tamaki N, Isobe H, Katayama T, Wada Y, Ohtoshi (2002) Delta-shaped anastomosis in totally lapariscopic Billroth I gastrectomy: new technique of intraabdominal gastroduodenostome. J Am Coll Surg 2: 284–287
Kida M, Watanabe M, Yamada Y, Tanabe S, Sakaguchi T, Koizumi W, Saigenji K (1999) Accuracy of endoscopic ultrasonography for diagnosis of the depth of early gastric cancer with or without ulcer fibrosis (with English summary). Stomach Intest 34:1095–1103
Kikuchi S, Katada N, Sakuramoto S, Kobayashi N, Shimao H, Watanabe M, Hiki Y (2004) Survival after surgical treatment of early gastric cancer: surgical techniques and long-term survival. Langenbeck Arch Surg 389: 69–74
Kikuchi S, Sakakibara Y, Sakuramoto S, Kobayashi N, Shimao H, Mieno H, Kato Y, Kadowaki K, Kakita A (2001) Recent results in the surgical treatment of gastric cancer according to the Japanese and TNM classification. Anticancer Res 21: 3589–3594
Kikuchi S, Sato M, Katada N, Sakuramoto S, Kobayashi N, Shimao H, Sakakibara Y, Kakita A (2000) Surgical outcome of node-positive early gastric cancer with particular reference to nodal status. Anticancer Res 20: 3695–3700
Kitano S, Iso Y, Moruyama M, Sugimachi K (1994) Laparoscopy-assisted Billroth I gastrectomy. Surg Laparosc Endosc 4: 146–148
Kitano S, Shiraishi N, Fujii K, Yasuda K, Inomata M, Asdachi Y (2002) A randomized controlled trial comparing open vs laparoscopy-assisted distal gastrectomy for the treatment of early gastric cancer: an interim report. Surgery 131: 306–311
Kojima K, Yamashita T, Inokuchi M, Sugihara K (2002) Technique of vagus-nerve sparing laparoscopy-assisted distal gastrectomy. Dig Endosc 14: 103–106
Mochiki E, Nakabayashi T, Kamimura H, Haga N, Asao T, Kuwano H (2002) Gastrointestinal recovery and outcome after laparoscopy-assisted versus conventional open distal gastrectomy for early gastric cancer. World J Surg 26: 1145–1149
Shiraishi N, Adachi Y, Kitano S, Bandoh T, katsuta T, Morimoto A (1999) Indication for and outcome of laparoscopy-assisted Billroth I gastrectomy. Br J Surg 86: 541–544
Tanabe S, Koizumi W, Mitomi H, Nakai H, Murakami S, Nagaba S, Kida M, Oida M, Saigenji K (2002) Clinical outcome of endoscopic aspiration mucosectomy for early stage gastric cancer. Gastrointest Endosc. 56: 708–713
Tanimura S, Higashino M, Fukunaga Y, Osugi H (2001) Hand-assisted laparoscopic distal gastrectomy with lesional lymph node dissection for gastric cancer. Surg Laparosc Endosc Percut 11: 155–160
Uyama I, Sugioka A, Fujita J, Komori Y, Matsui H, Soga R, Wakayama A, Okamoto K, Ohyama A, Hasumi A (1999) Completely laparoscopic extragastric lymph node dissection for gastric malignancies lacated in the middle or lower third of the stomach. Gastric Cancer 2: 186–196
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Sakuramoto, S., Kikuchi, S., Kuroyama, S. et al. Laparoscopy-assisted distal gastrectomy for early gastric cancer. Surg Endosc 20, 55–60 (2006). https://doi.org/10.1007/s00464-005-0126-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-005-0126-5