Abstract
Purpose
The diatomic radical nitric oxide (NO) has been the cause of intense debate with implication in carcinogenesis, tumour progression, invasion, angiogenesis and modulation of therapeutic responses. The tumour biology of NO is highly complex, and this review summarises the various protective and damaging mode of action of NO.
Methods
We reviewed all published literature addressing the complexities of the role of NO in the altered biology of cancer and evaluating promising therapeutic roles of NO/iNOS for anti-cancer therapy.
Results
The available experimental evidences highlight contrasting pro- and anti-tumour effects of iNOS expression, which appear to be reconciled by consideration of the concentrations of NO involved, the temporo-spatial mode of NO action, intracellular targets, cellular redox state and the timing of an apoptotic stimulus. Several clinical and experimental studies indicate that the presence of NO in tumour microenvironment is detrimental to tumour cell survival and metastasis. In contrast, numerous reports suggest that NO can have tumour-promoting effects. NO is a ‘double-edged sword’ in cancer, and this review offers insight into the dichotomous nature of NO and discuss the therapeutic gain that can be achieved by manipulating tumour NO.
Conclusions
NO may exert a biphasic response, such that when NO levels go beyond a critical concentration that would be suitable for tumour growth and survival, growth arrest and/or apoptotic pathways are initiated. These characteristics of NO have been exploited therapeutically with impressive effects in pre-clinical models of cancer to slow tumour growth and to enhance the efficacy of both chemotherapy and radiotherapy.
Similar content being viewed by others
Introduction
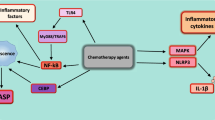
Biosynthesis of nitric oxide (NO) is catalysed by a family of enzymes called NO synthases (NOS). NOS are dimeric enzymes with each monomer composed of two distinct catalytic domains: NH2-terminal oxygenase domain and COOH-terminal reductase domain. N-terminal is the binding site for heme 5,6,7,8-tetrahydrobiopterin (BH4), oxygen and l-arginine, whereas NADPH, FMN and FAD bind on C-terminal [1]. The catalytic mechanisms of NOS involve flavin-mediated electron transport from NADPH to the heme centre, where oxygen is reduced and incorporated into the guanidine nitrogen of l-arginine producing NO and L-citrulline [2] (Fig. 1). Three distinct isoforms of the enzyme NOS have been reported; neuronal NOS (nNOS or NOSI), inducible (iNOS or NOSII) and endothelial NOS (eNOS or NOSIII). The three isoforms share about 50% sequence homology and are differentially regulated making the catalytic activity distinct for each isoform. The eNOS and nNOS isoforms are constitutive and calcium/calmodulin-dependent and generate NO in the picomolar–nanomolar range for short periods of time. The iNOS isoform is induced by cytokines and is not dependent upon calcium/calmodulin for its enzymatic action. iNOS is expressed in essentially every cell type and can locally generate high output quantities of NO at micromolar range for prolonged periods of time [1]. Beside these three isoforms, a mitochondrial-specific NOS (mtNOS) has also been recently described, which has important implications for the role of NO in mitochondrial bioenergetics [3]. NO is an uncharged molecule containing an unpaired electron that allow it to react with inorganic molecules (i.e. oxygen, superoxide or transition metals), structures in DNA, prosthetic groups (i.e. heme) or with proteins and, thus responsible for its complex and pleiotropic biological activity [4]. Evidences are accumulating for the role of NO as an oncopreventive agent and more recently as a novel therapeutic to overcome tumour cell resistance.
NO chemistry of biological significance. NO is synthesised endogenously from l-arginine, NADPH and oxygen. NO freely diffuses creating concentration gradients across subcellular compartments. Redox or additive reactions with constituents of cellular microenvironment convert NO to a number of NOx species, which in turn, dictate the biological effects of NO
Regulation of iNOS Activity
The induction of iNOS and the subsequent biological actions of NO are complex mechanisms that may partly explain the contradicting results in NO biology obtained by different groups. Extensive in vitro studies using macrophages and cancer cell lines have shown that three major pro-inflammatory cytokines induce iNOS; these are the interleukin-1s (IL-1s), tumour necrosis factor-α (TNF-α) and interferon-γ (IFN-γ) [5]. TNF-α, IL-1β or endotoxins, such as lipopolysaccharide stimulate iNOS transcription by activation of the transcription factor nuclear factor κB (NF-κB), which binds to κB element in the NOS promoter [5]. Similarly, IFN-γ activates the transcription factor interferon regulatory factor-1 (IRF-1), which also binds to the NOS promoter [6]. Maximal induction of the iNOS gene requires physical interaction between NF-κB and IRF-1 while bound to the NOS promoter.
HIF-responsive element (HRE) is also present in the NOS promoter, which can promote transcriptional induction under hypoxia [7]. Tumours are hypoxic, and iNOS can be induced through synergism between IRF-1 and hypoxia inducible factor-1 (HIF-1) [8]. Besides hypoxia, another important component of the disordered tumour microenvironment is high-mobility group box 1 (HMGB1) protein. HMGB1 is passively released from necrotic cells and actively released from inflammatory cells [9]. It binds with high affinity to several receptors including the receptor for advanced glycation end products (RAGE) and toll-like receptors (TLR)-2, TLR-4, TLR-9, thereby promoting inflammation [10]. In the case of tumours, HMGB1 recognition has a paradoxical dual effect as it not only promotes tumour neoangiogenesis but also triggers protective anti-neoplastic T cell responses [9]. RAGE activation induces cell growth through mitogen-activated protein kinase (MAPK) signaling [11] and is associated with induction of iNOS, NF-κB and B-cell lymphoma (Bcl-2) protein [12]. HMGB1 also has partial effects on the upregulation of iNOS and NF-κB expression [13]. Together, this suggests a complex regulation of iNOS gene expression by various signalling pathways.
Expression of iNOS in human tumours
During the last two decades, iNOS has been reported to be associated with several human malignant tumours including breast [14], brain [15], lung [16], prostate [17], colorectal [18] and pancreatic carcinomas [19], Kaposi’s sarcoma [20] and melanoma [21]. The first report of iNOS expression in human gynaecological tumours showed predominantly localised expression in tumour cells and lack of any detectable activity in normal tissue suggesting a relationship between iNOS activity and malignancy [22]. Subsequent studies showed a strong correlation between iNOS expression and higher tumour grade in malignant neoplasms of the central nervous system [15]. Immunohistochemical staining of these tumours showed iNOS to be localised primarily in areas between viable and necrotic regions of the tumour (an area that is presumably hypoxic). Furthermore, clinical observation indicates that patients with iNOS-expressing melanomas had significantly poorer survival rates than their iNOS-negative counterparts [21]. On the contrary, another group studied lymph nodes and subcutaneous metastases from melanoma patients and reported that patients with a lower percentage of iNOS-expressing tumour cells had a greater risk of developing distant metastases [23]. This dichotomy may be due to variation in the levels of NO, expression of pro- and anti-apoptotic genes and the presence of other reactive molecules. One of the large-scale breast cancer studies demonstrated that while none of the benign lesions had any detectable iNOS (0/41), 77% in situ carcinomas (21/27) and 61% invasive lesions (33/54) showed iNOS tumour cell staining [24]. Taken together, these studies indicate that in order to determine the precise function(s) of NO in tumour cell biology, understanding of the enzyme’s activity and a clear identification of iNOS localisation in tumour and stromal tissues is required.
Role of eNOS in cancer
Multiple clinical observations indicate that eNOS is not only expressed in normal tissue, but also extensively expressed in tumour tissues. eNOS is relevant in tumour progression, as it has been shown to modulate cancer-related events like angiogenesis, apoptosis, cell cycle, invasion and metastasis [25]. Although iNOS remains a viable candidate for purposes of cancer prevention and treatment, studies suggest that targeting eNOS may also be a viable strategy. In addition to tumour cell expression, eNOS is particularly expressed by vascular endothelial cells or surrounding stromal cells and therefore has been a focus of attention in angiogenesis. Vakkala et al. [26] reported that eNOS was expressed in 65% of invasive breast carcinoma samples with immunopositivity seen both in stromal structures and carcinoma cells. In another study, the positive expression rate of eNOS was 89% in non-small cell lung cancer tissues [27]. Knockdown of the eNOS gene or selective inhibition of eNOS by L-NG-nitroarginine methylester (L-NAME) inhibited the homing of peripheral endothelial progenitor cells and neoangiogenesis in tumours, demonstrating that NO promoted neoangiogenesis [28]. Multiple hormone agonists such as bradykinin, estradiol and vascular endothelial growth factor (VEGF) induce eNOS expression in tumour cells in association with elevations in cytosolic calcium concentrations [29]. In contrast, eNOS activation by shear stress and isometric vessel contraction occurs independently of changes in intracellular calcium levels [30]. eNOS and associated NO can increase the permeability of the tumour–blood barrier and therefore may play a role in tumour invasion. Clinical studies suggest that high eNOS expression can be positively correlated with vascular invasion in human gastric cancer [31] and trophoblastic disease [32].
In addition to regulatory pathways involving calcium/calmodulin, the dynamic regulation of eNOS involves numerous pathways of phosphorylation and dephosphorylation. All NOS isoforms are subject to regulation by phosphorylation. eNOS is known to be phosphorylated at multiple sites, including Ser 1177 and Ser 635, which are stimulatory and Thr 495 and Ser 116, which are inhibitory [33]. Protein kinases that modify eNOS activity include AMP-activated protein kinase (PKC), cAMP-dependent protein kinase (PKA) and the serine/threonine kinase Akt [34]. There is evidence of coordinated regulation of eNOS activity by agonists such as VEGF, which cause both phosphorylation of Ser 1177 and dephosphorylation of Thr 497 [35]. Furthermore, VEGF increases angiogenesis in both iNOS +/+ and iNOS–/– mice but not in eNOS–/– mice, supporting a predominant role of eNOS in VEGF-induced angiogenesis and vascular permeability [36]. Recent work has further demonstrated that PKA signaling leads to eNOS phosphorylation at Ser 1177 and dephosphorylation of Thr 497, thereby enhancing enzymatic activity, whereas PKC promotes the dephosphorylation of Ser 1177 and the phosphorylation at Thr 497, resulting in attenuated enzyme activity [37]. eNOS activity is regulated by a complex combination of protein–protein interactions and signal transduction cascades involving calcium mobilisation and phosphorylation events. Thus, it is possible that the NO generated from this activation of eNOS may contribute significantly to tumour cell survival under hypoxia and other stress conditions.
cGMP-dependent and cGMP-independent signalling
The pro-tumourigenic versus anti-tumourigenic effect of NO depends on the cellular makeup, surrounding microenvironment (e.g. other inflammatory species and free radicals), the activity and localisation of NOS isoforms and overall levels. Nitric oxide production kinetics by iNOS differ greatly from the production by eNOS or nNOS. iNOS produces very large, toxic amounts of NO in a sustained manner, whereas constitutive NOS isoforms produce NO within seconds and its activities are direct and short acting. Low levels of NO produced by constitutive synthases primarily interact directly with positively charged metal ions of guanylate cyclase (sGC), cytochrome C oxidase, cytochrome p450 and NOS itself [37]. NO activates sGC cyclase leading to the synthesis of cyclic guanosine monophosphate (cGMP) from guanosine triphosphate (GTP). This in turn depletes intracellular Ca2+ levels by reducing Ca2+ release from intracellular stores, Ca2+ influx and Ca2+ uptake mediated by calcium adenosine 5-triphosphatase of the endoplasmic reticulum [37]. These actions thereby stimulate muscle relaxation, increase vascular permeability and exert anti-proliferative, anti-platelet and anti-oxidant effects through cellular targeting of downstream effectors (i.e. protein kinases, phosphodiesterases and ion channels) [38]. Recent data have also indicated that NO produced by constitutive NOS enzymes may be involved in immune regulation of T helper cell proliferation and cytokine production [39]. NO formed by eNOS seems to be mostly cytoprotective, possibly due to its characteristic redox properties [38].
Cytochrome C oxidase, which reduces oxygen and pumps protons across the inner mitochondrial membrane, generating the potential that drives ATP synthesis, is inhibited by NO binding to its oxygen-binding site [39]. Inhibition of oxygen consumption by NO is postulated to modulate cellular function under physiological conditions. Endothelium-derived NO may increase permeation of oxygen into the tissue, inhibiting oxygen consumption near blood vessel walls so that oxygen is available to diffuse to more distant regions [40]. NO produced physiologically by nNOS and eNOS does not reach concentrations at which it can significantly inhibit respiration. Instead, in normoxic conditions, it is present at only 0.6–1.1 nM, a concentration range that is within the sensitivity range for sGC but not for cytochrome C oxidase [41]. In pathological situations, such as ischaemia or inflammatory conditions when iNOS is expressed, it is more likely that increased free radical generation, rather than compromised oxygen consumption, is responsible for iNOS-mediated cell damage. NO at higher concentrations combines with other oxidants to from reactive nitrogen species (RNS), which can damage a variety of cellular targets such as DNA and proteins, ultimately leading to apoptosis and mutagenesis [37]. When NO interacts with oxygen and superoxide (O2 −), nitrosylation and nitration occur, respectively. With respect to nitrosylation, NO interact with oxygen, electron acceptors or metals to produce nitrosonium ion (NO+), which can subsequently interact with thiols such as cysteine residues in proteins. Similarly, NO interact with O2 − to generate peroxynitrite (ONOO−), which leads to tyrosine nitration of proteins [37]. This chemistry of NO facilitates its interaction with several proteins, thus regulating various intracellular and intercellular signalling events.
Another important variable of these distinct concentration gradients relative to their biologic response is the enzymatic activity of specific NOS isoforms. Two of the isoforms, nNOS and eNOS, are controlled by calcium influx, which generates a burst of 10–50 nM NO lasting only minutes [42]. However, phosphorylation of eNOS removes the calcium dependence and prolongs the production of NO [42]. iNOS-expressing cells generate NO for prolonged periods, which can range from high (300 nM) to low (<100 nM) levels, depending on the inducing cytokines and inflammatory mediators [42]. In vivo NO fluxes are controlled specifically and in addition to rate of synthesis and NO concentration, the biologic outcome also depends on cellular consumption and the redox environment. These discrete NO-signalling profiles suggest that NO concentration can be finely tuned to elicit different biologic responses, which has recently been extended by studies identifying an NO biphasic angiogenic response [43].
Post-translational modifications induced by NO
Post-translational modifications of proteins by NO represent mechanisms through which it may regulate cellular signalling in carcinogenesis and cancer chemotherapy treatment. These post-translational modifications induced by high intracellular levels of NO include nitrosylation of thiol and amine groups; nitration of tyrosine, tryptophan, amine, carboxylic acid and phenylalanine groups and oxidation of thiols and tyrosine [44] (Fig. 1).
S-Nitrosylation
S-nitrosylation is the reversible coupling of a NO moiety to a sulfur atom to form S-nitrosothiol (RSNO), and unlike phosphorylation or ubiquitinylation, it is not enzyme-dependent [44]. The propensity of certain cysteine residues to get nitrosylated or de-nitrosylated depends upon a number of factors including the electrostatic environment, orientation of aromatic residues, hydrophobicity, protein–protein interactions and the redox microenvironment regulated by the NADPH/NADP+, GSH/GSSG couples, the thioredoxin (Trx) system and others enzymes [44]. Molecular alterations that lead to apoptosis resistance can be initiated or promoted by S-nitrosylation. For example, apoptosis signal regulating kinase 1 (ASK1) is inhibited by S-nitrosylation of its cysteine-869 residue, thus inhibiting apoptosis [45]. Meanwhile, activation of ASK1 was observed in human embryonic kidney HEK293 cells by S-nitrosylation of Trx protein [46]. Also, NO inhibits the function of NF-κB [47], protein kinase C (PKC) [48] and c-Jun N-terminal kinase (JNK) [49] and activates Ras [50] and ryanodine receptor [51] via S-nitrosylation.
Tyrosine nitration
Tyrosine nitration is incorporation of a nitro group (–NO2), generally at position 3 of the phenolic ring of a tyrosine residue yielding 3-nitrotyrosine [44]. There are two main mechanisms leading to tyrosine nitration in vivo, the formation of peroxynitrite and the production of nitrogen dioxide (NO2). Nitration of tyrosine residues can block protein phosphorylation by interfering with tyrosine residues, thus modifying cell signalling pathways. MacMillan–Crow et al. [52] showed that exposure of the pancreatic ductal adenocarcinoma cells to ONOO− induces c-Src tyrosine kinase nitration and phosphorylation, thus increasing c-Src activity and cell growth.
S-Glutathionylation
The GSH/GSSG redox system maintains cellular proteins in a reduced state. The main form of glutathione is the reduced form (GSH), whereas only less than 2% of glutathione is present in oxidised glutathione disulfide form (GSSG) [53]. Normally, S-nitrosylated proteins are rapidly reduced by GSH, which in turn could be S-nitrosylated to nitrosoglutathione (GSNO) [44]. GSNO is an effective agent for the direct transfer of NO to other thiols, including proteins, by transnitrosylation. In addition, glutathione could potentially replace the NO on S-nitrosylated proteins, converting the proteins to an S-glutathiolated form via reversible disulfide bonds, and thus dynamically regulating the protein function [53].
NO: cellular signalling and concentration dependence
Many of the biological and pathological effects of NO are mediated through cell signalling pathways. Reports demonstrated that shear stress induces the formation of NO and activates the stress-activated protein kinase/c-Jun N-terminal kinase (SAPK/JNK) and MAP kinase, extracellular signal-regulated protein kinase (ERK) [54]. Activation of the different MAPK cascades by NO may occur either by direct alterations to the kinases themselves or by modulation of an upstream factor, such as a GTP-binding protein p21ras [55]. Also, NO directly modulates the Janus kinases (JAKs)/signal transducer and activator of transcription (STAT) [56] and PI3 K-Akt [57] signalling pathway. Both JAK2 and JAK3 autokinase activity have been found to be inhibited by NO, presumably by oxidation of crucial thiols to disulphides [56]. These cascade events then trigger the phosphorylation of key nuclear proteins, including transcription factors such as c-Jun, leading to alterations in gene expression [58].
Due to its lipophilic nature, NO can rapidly cross cell membranes and enter intracellular compartments, where it can exert its action even when produced by a neighbouring cell (tumour or stromal cells) within the tumour and endothelial cells in the tumour microvasculature, thus mediating interactions between tumour and host cells [59]. Tumour cells have quite different NO concentration requirements to cause either a pro-growth or an anti-growth phenotype. Characterising steady state of NO is, therefore, of particular importance when assessing its effects at the cellular level. MCF7 breast cancer cells were found to activate specific signalling pathways in response to distinct fluxes of NO [60]. Low levels of NO (<50 nM) were associated with increased cGMP-mediated ERK phosphorylation and intermediate levels (>100 nM) lead to HIF-1α stabilization. However, the pro-survival effects of NO are lost at high NO concentrations (>400 nM), which is signified by increases in phosphorylation of tumour suppressor protein p53 [61]. Pervin et al. [62] showed that treatment for breast cancer cells with NO donor diethylenetriamine-NONOate (DETA/NO) (30–60 μM), led to increased pAkt and pERK, and interruption of ERK and Akt phosphorylation inhibited proliferation of these cells. Furthermore, prolonged exposure of breast cancer cells to 1 mM DETA/NO for an extended period of time resulted in MAP kinase phosphatase-1 (MKP1)-mediated pERK and pAkt dephosphorylation with subsequent induction of apoptosis. Though NO is short lived, the sustained NO flux generated by iNOS can vary in duration from seconds to days, thus deciding the anti-apoptotic/pro-apoptotic effects of NO.
Molecular effects of NO on apoptosis
Increasing amount of evidences suggest that iNOS has the potential to produce NO at toxic levels that may be exploited in achieving direct apoptosis. NO induces apoptosis through heme nitrosylation of cytochrome c, which enhances its pro-apoptotic function, leading to increased caspase-3 activation [63]. NO can activate other apoptotic pathways independent of caspase activation or perhaps activate other caspases, not commonly involved in apoptosis. For instance, NO donor glyceryltrinitrate is able to induce apoptosis in human colon cancer cells by activation of caspases-1 and -10 [64]. In contrast, nitrosylation of caspases-8, -9 and -3 at their active sites has been shown to inhibit their enzymatic activity [65]. Long-term exposure of non-tumourigenic lung epithelial cells to non-toxic concentrations of carcinogenic metal Cr(VI) led to apoptosis resistant and malignant transformed phenotype. These cells exhibited increased NO production and elevated expression of S-nitrosylated Bcl-2, which was accompanied by a parallel increase in total Bcl-2 level, suggesting positive regulation of Bcl-2 by S-nitrosylation through protein stabilization [66]. S-nitrosylation of these proteins precludes their ubiquitination and subsequent degradation by the proteasome, thus accentuating their anti-apoptotic effect that is critical in the context of tumourigenic potential and cancer progression. Since resistance to apoptosis is a hallmark of neoplastic evolution, selection of cells that are resistant to apoptotic cell death by S-nitrosylation may be a key determining factor in cancer progression.
Another important facet of the potential apoptotic mechanism of NO is the regulation of p53. Activation of the transcription factor p53 was shown to play a role, since the synergy between NO and radiation was decreased in tumours induced by p53-mutated cells [67]. The introduction of p53 gene into cells lacking functional p53 enhanced the synergy, which was due to the phosphorylation of p53 on serine 15 [68]. In a subsequent report, it was shown that GSNO enhanced markedly the ability of low-dose ionising radiation to elicit apoptotic killing of human neuroblastoma cells expressing cytoplasmic wild-type p53 [69]. NO induced the phosphorylation of p53 in these cells via the kinase ATR (ataxia telangiectasia and Rad3 related) and promoted p53 nuclear retention [70]. A strong correlation between p53 phosphorylation and iNOS protein expression in human samples of ulcerative colitis provided further evidence that NO activate p53 pathway in vivo [71]. Other studies have demonstrated that in human malignant cell lines, this is a low-dose effect of NO, whereas high NO concentrations leading to peroxynitrite formation can inactivate p53 by tyrosine nitration [72]. This would explain the inactivation of the p53 pathway found in tumours lacking p53 gene mutations.
Moreover, NO may modulate tumour DNA repair mechanisms by up-regulating poly(ADP-ribose) polymerase (PARP) and the DNA-dependent protein kinase (DNA-PK) [73]. Several kinases including PKC, ERK and activator protein-1 (AP1) were inhibited at high concentrations of S-nitroso-N-acetylpenicillamine (SNAP) and up-regulated at low concentrations [74]. NO also induces the expression of MKP-1 leading to dephosphorylation of ERK, which is the initial and essential step that commits cancer cells to programmed cell death [75]. Apoptosis can also be promoted by NO via down-regulation of expression of anti-apoptotic protein survivin, as observed in human lung carcinoma cells [76]. NO also up-regulates Fas expression in ovarian carcinoma cell lines through the specific inactivation of the transcription repressor yin-yang-1, which binds to the silencer region of the Fas promoter [77]. Moreover, NO sensitises human ovarian carcinoma and prostatic adenocarcinoma cells to TNF-α-mediated apoptosis through the specific disruption of the TNF-α-induced generation of hydrogen peroxide, inhibiting the activity of the NF-κB and consequently the impaired expression of the anti-apoptotic genes [78].
NO as a promoter of tumour growth
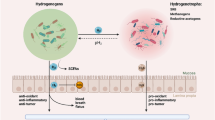
To date, much conflicting data have been presented, which highlight both pro- and anti-tumour effects evoked by NO (Fig. 2). Inhibition of tumour growth, via the selected restriction of the tumour vasculature using NOS inhibitors, led to the initial hypothesis for the supportive role of NO expression in cancer progression. Tozer et al. [79] demonstrated that NOS inhibitor, NG-nitro-l-arginine (L-NNA) at dosage of 1 mg/kg, significantly reduced tumour blood flow and increased vascular resistance within the tumour without causing any significant vascular changes in normal tissues. Ishii et al. [80] reported that NO generation may promote tumour progression through the activation of various matrix metalloproteinases (MMP). In human melanoma C32TG cells, MMP-1, -3, -10 and -13 were transcriptionally enhanced when exposed to increasing doses of NO donor SNAP. Further investigation confirmed that MMP-1 activation was transcriptionally enhanced by NO via the ERK and p38 MAPK pathways, and that these pathways were highly activated during tumour inflammation, resulting in tumour progression [81].
Balancing cell death and survival: Role of NO. Several factors that can tip the balance towards pro- versus anti-apoptotic actions of NO are shown. The sum of these variables at the end will regulate cellular susceptibility towards NO and RNS and dictate whether they exert pro- or anti-tumour effects
The elevated NO release within a tumour has also been shown to result in the overproduction of VEGF. Previous studies have strongly correlated the up-regulation of VEGF-C with higher metastatic potential and poorer prognosis [82]. NO donor drug DETA-NONOate significantly increased VEGF-C expression in breast cancer cells. This was further confirmed when the increases noted were inhibited in the presence of L-NAME, suggesting that VEGF-C expression is at least in part controlled by NO [83]. Similarly, in human gastric carcinoma specimens, iNOS expression levels were found to correlate with both VEGF levels and microvessel density [84]. The therapeutic activity of anti-VEGF monoclonal antibody, bevacizumab, recently approved for patients with colorectal cancer is associated with inhibition of NO production [85]. An in vitro assay, which examined tubule formation and the activity of several mechanistic processes, involved in angiogenesis showed that lower concentrations of SNAP (0.1–0.3 mM) significantly increased angiogenesis by up to 46%; at progressively higher concentrations, the pro-angiogenic effects started to diminish, and at a SNAP concentration of 4 mM, a maximal angiogenesis inhibition of 80% was observed [74]. This clearly demonstrates the dose-dependent response to NO with regard to angiogenesis. Another mechanism by which NO may promote tumour growth is by activating cyclooxygenase-2 (COX-2), which by modulating the production of prostaglandins promotes angiogenesis and inhibits apoptosis [86].
NO as an inhibitor of tumour growth
The first report of anti-tumour potential evoked by expression of the iNOS enzyme was in a human colorectal adenocarcinoma cell line. Cells from both the primary tumour SW480 and from lymph node SW620 metastases were shown to express calcium-independent NOS activity [87]. Inhibition of this activity using the NOS inhibitor NG-monomethyl-l-arginine (NMLA) subsequently increased the metastatic potential of the SW480 cells to the same level as that of the SW620 cells. Comparison studies between the characteristics of several non-metastatic and highly metastatic clones, produced from an original K1735 melanoma, revealed that the non-metastatic clones generally expressed much higher levels of endogenous NO [88]. Xie et al. [89] preformed a series of transfection studies where mice implanted with the highly metastatic K1735 cell line were treated with either a functional iNOS gene or an inactive muted iNOS gene. The control group and the group transfected with the muted iNOS gene developed into highly metastatic aggressive tumours, whereas the tumours transfected with the functional iNOS gene produced slow growing tumours, which were not metastatic.
Le et al. [90] reported anti-tumour effects resulting from the over expression of NO, whilst at the same time noting that the pro-tumour and pro-angiogenic factors, VEGF and IL-8 were up-regulated in human pancreatic cells transfected with the iNOS gene. This suggests that the anti-tumour effects generated by over production of NO outweigh the pro-tumour effects of up-regulation of VEGF and IL-8, resulting in an overall net anti-tumour effect. If this is the case, specialised sub-colonies of NO-resistant cells may survive, which will have a stronger tumourigenic and metastatic potential. Systemic delivery of NO donor drugs at high concentration results in hypotension, but one class of agent, the glutathione S-transferase activated NO pro-drugs has shown some promise for NO therapy of cancer. Intravenous injection of one such agent, JS-K [O 2-(2,4-dinitrophenyl) 1-[(4-ethoxycarbonyl) piperazin-1-yl]diazen-1-ium-1,2-diolate], into mice bearing subcutaneously implanted multiple myeloma tumours, resulted in tumour growth delay and induction of extensive apoptosis throughout the tumour [91].
NO-mediated chemosensitisation of tumours
NO has been found to be a pivotal factor in the chemosensitisation of tumour cells to various chemotherapeutic drugs. In human breast carcinoma MDA231 and mouse melanoma B16F10 cells, inhibition of NO enhanced hypoxia-induced chemoresistance, suggesting that hypoxia-mediated drug resistance is likely a result of suppression of endogenous NO production and that NO functions as a chemosensitiser in tumour cells [92]. Konovalova et al. [93] showed that in leukaemic mice, co-injection of cyclophosphamide and NO donor significantly increased cyclophosphamide activity and inhibited metastasis. A separate study showed an analogous role for NO in chemosensitisation through the use of a doxorubicin resistant epithelial colon cell line (HT29-dx). Administration of NO donor SNAP reversed the resistance of HT29-dx cells to doxorubicin by triggering tyrosine nitration of multidrug resistant-associated proteins, thus reducing the number of P-glycoprotein transporters and inhibiting the efflux of doxorubicin [94].
NO donors DETA/NO and GTN decreased the resistance of doxorubicin by 33–50% in human breast carcinoma cells cultured as spheroids [95]. Supporting this, DEA/NO and DETA/NO increased the cytotoxicity of melphalan and fludarabine in human breast carcinoma cells and B-cell lymphocytic leukaemia cells, respectively [96, 97]. In a phase II trial, Yasuda et al. [98] investigated the efficacy and safety of GTN plus vinorelbine and cisplatin in 120 patients with previously untreated stage IIIB/IV non-small-cell lung cancer. The study showed that treatment with GTN improved the response rate, time to disease progression and survival in patients with advanced cancer, without major adverse effects. These data suggest that NO can be used as a chemosensitising agent, and combination treatment of NO donors and chemotherapy may result in synergistic activity in the treatment for cancer.
Effect of NO on the expression and activity of HIF-1α
The mechanisms involved in cancer and cancer treatment are diverse and tumour hypoxia is a primary reason for treatment failure. Hypoxia not only limits the effects of radiation but due to greater diffusion distances also reduce the effectiveness of most anti-cancer drugs [99]. HIF-1 contributes to drug resistance by increasing genetic instability, altering cellular metabolism and down-regulating pro-apoptotic proteins [100]. HIF-1 also increases the expression of iNOS and in a positive-feedback circuit, NO activate HIF-1. Several studies reported the accumulation of HIF-1α and increased HIF-1 activity under the influence of NO in aerobic conditions (21% oxygen) [101]. The inhibition of prolyl hydroxylase (PHD) activity by NO and activation of the PI3 K-Akt pathway were suggested to be involved in the regulation of HIF-1α stabilization by NO under these conditions [102]. Using a cell line engineered to generate NO (driven by a tetracycline promoter), it has been shown that low (physiologic) levels of NO (concentrations up to 400 nM) under hypoxic conditions inhibit mitochondrial respiration, diverting the available oxygen to PHDs. As a result, cells fail to detect hypoxia and subsequently result in degradation of HIF-1α. In contrast, high (pathologic) concentration of NO (>1 μM) stabilized HIF-1α expression in a mitochondria-independent manner under similar hypoxic conditions, as well as under non-hypoxic conditions [103]. It has been postulated that high levels of NO within the tumour microenvironment might have the same effect as hypoxia in inducing angiogenesis. Despite all the problems associated with hypoxia, these regions are a unique feature of solid tumours that do not occur in normal tissues so can potentially be exploited in cancer therapy.
iNOS-dependent activation of bioreductive drugs
To circumvent hypoxia-related resistance to therapy, class of drugs known as bioreductive pro-drugs have been developed [104]. These non-toxic pro-drugs are substrate for intracellular reductase enzymes (e.g. cytochrome P-450 reductase, cytochrome-b 5 reductase, DT-diaphorase, iNOS reductase), which add an electron to the pro-drug, converting it to a toxic radical species in hypoxic conditions [105]. Tirapazamine (TPZ, 3-amino-1,2,4-benzotriazine-1,4-dioxide; Fig. 3) was one of the first compounds to show selective hypoxic cytotoxicity [105]. TPZ is activated in hypoxia by one-electron reductases to form the free radical TPZ· that undergoes spontaneous decay to an oxidising hydroxyl radical (OH·) and an oxidising benzotriazinyl radical (BTZ·) [104, 106]. Stratford and co-workers [107] investigated the role of iNOS in the bioactivation of TPZ by constitutively overexpressing the iNOS gene in human breast adenocarcinoma cells. They showed that an increase in iNOS activity in a series of transfected clones corresponded with an increase in TPZ metabolism and toxicity under hypoxic conditions. iNOS-mediated reduction of TPZ resulted in a significant increase in DNA damage in hypoxia without any increase in aerobic toxicity.
iNOS-based therapeutic strategy against cancer. Reductase domain of iNOS can activate bioreductive drugs in the absence of oxygen and oxygenase domain generate high concentrations of NO, which act as a direct cytotoxic as well as a potent radiosensitiser. Diffusion of NO and activated bioreductive drugs to neighbouring cells can further exert a strong bystander effect
Another bioreductive agent suggested to be activated by iNOS is the di-N-oxide analogue of mitoxantrone [1,4-bis{2-(dimethylamino-N-oxide) ethylamino}5,8-dihydroxy-anthracene-9,10-dione; Banoxantrone; AQ4 N; Fig. 3] [108]. AQ4 N undergoes an oxygen-dependent 2e− reduction to the mono-N-oxide intermediate AQM before a further oxygen-dependent 2e− reduction to form the toxic product AQ4 [104]. Bioactivation of AQ4 N may sensitise tumours to radiotherapy and chemotherapeutic agents by inhibiting topoisomerase [108]. Preliminary studies demonstrate that adenoviral delivery of iNOS can enhance hypoxic tumour response to AQ4 N and radiation [109]. The ability of iNOS to activate bioreductive drugs and its capacity to generate the radiosensitiser NO will, therefore, make it a suitable enzyme pro-drug therapy in combination with radiation (Fig. 3).
Tumour radiosensitisation through NO
Ionising radiations are used as first-line therapy in malignancies, including breast, head and neck, colorectal, lung and oesophageal cancers [110]. The role of NO as a radiosensitiser was first reported in hypoxic bacteria and human cells 5 decades ago, however, its tumour radiosensitising potential has recently been realised [111, 112]. Studies showed that NO released by donor drugs increased the radiosensitivity of human tumour cells grown in hypoxic conditions in vitro [113]. Recently, Wardman et al. [114] showed that NO at 40 ppm caused significant radiosensitisation of anoxic V79 cells, whereas similar concentrations of oxygen had barely detectable radiosensitisation, suggesting that NO is an even more potent radiosensitiser than oxygen. Moreover, chemical features of NO include its rapid diffusion from the point of synthesis (the diffusion coefficient is 1.4 times that of oxygen at 37°C).
Intratumoural oxygen concentration is highly variable (0.01–3% oxygen) and thus can influence the outcome of radiotherapy. Much of the work involving endogenous NO that is generated in tumour cells by iNOS or NO donor drugs has been done without taking account of the contribution of intermediate oxygen concentrations. To evaluate this, Singh et al. [115] demonstrated that under low-oxygen conditions (<0.01% oxygen), activation of iNOS by cytokines was not accompanied by release of NO (since oxygen is required for the generation of NO). As a consequence, when these cells were irradiated, no radiosensitisation was observed. However, as the oxygen levels were increased, the amount of NO generated also increased, and this NO then contributed to an overall increase in the radiosensitivity of cells. NO did not further enhance the radiosensitivity of cells in normoxia (5% oxygen) and aerobic conditions (21% oxygen), indicating that NO acts as a radiosensitiser at low to intermediate oxygen levels and would not affect the sensitivity of normal aerobic cells to radiation. Li et al. [116] demonstrated that radiation itself can directly stimulate iNOS expression and subsequent NO production by tumour-associated macrophages activate HIF-1α in the surrounding tumour cells. It is possible that radiation-induced reoxygenation of the hypoxic regions of the tumours leads to increased oxygen availability in these regions and subsequent NO generation in cells that already overexpress iNOS. Targeting tumours exhibiting high levels of endogenous NO production with radiation and HIF-1 inhibition are a potential strategy to counteract the radioprotective effects of HIF-1 by shifting the balance towards apoptosis.
iNOS-based suicide gene therapy
Despite the fact that NO is a promising radiosensitiser, non-specific generation of NO in vivo through the systemic use of NO donors is faced with complications. The application of NO donors at sufficient doses to cause significant tumour radiosensitisation may result in intolerable systemic effects such as hypotension, limiting their application in the clinic [117]. Several strategies have been suggested in an attempt to achieve a more specific and localised expression of the iNOS gene. The potential for iNOS in a suicide gene therapy approach was first demonstrated by Soler et al. [118], who showed a strong anti-tumour effect in a rat model of human medullary thyroid carcinoma using a naked iNOS plasmid driven by the cytomegalovirus (CMV) promoter. Xie and co-workers [90] used adenoviral vectors containing the mutated iNOS gene to examine the effects of iNOS gene therapy on tumour growth and metastasis. Depending upon the levels of enzymatic activity, NO was generated at different levels in tumour cells, which directly correlated with the in vitro and in vivo anti-tumour activity. Furthermore, intratumoural injections of an adenoviral vector carrying iNOS gene in HCT116 and SNU1040 human colon cancer xenografts in mice resulted in impressive inhibition of tumour growth compared to radiation alone [119].
Hirst and colleagues [120] used cationic lipid vectors to deliver the iNOS gene driven by radiation inducible promoter, wild-type activating fragment-1 (WAF1) in HT29 colorectal adenocarcinoma xenografts in SCID mice. Under hypoxic conditions, the WAF1/iNOS gene therapy achieved a higher sensitiser enhancement ratio when combined with a 20 Gy dose of X-rays, highlighting the potential therapeutic benefit of iNOS gene therapy in tumours generally regarded as radioresistant. To further evaluate the potential of iNOS gene therapy in a clinical setting, RIF1 and HT29 tumour-bearing mice were given a course of iNOS gene therapy and fractionated radiation doses. Highly significant growth delays were observed in both the RIF1 and HT29 tumours, indicating significant targeted radiosensitisation by WAF1/iNOS gene therapy. Together, these studies confirm that systemically delivery of iNOS gene have potential for achieving substantial anti-tumour effects.
In the search for new oncotherapies, many groups have harnessed the potent anticancer nature of NO. The low NO flux in tumours mainly, though not exclusively plays a key role in maintaining the malignant phenotype. Studies indicate that inhibition of NO production consistently reduced the rate of tumour growth, but was unable to prevent growth entirely. In addition, iNOS inhibition created a poorly perfused, hypoxic environment, which could be exploited to enhance the cytotoxicity of bioreductive drugs, but would be detrimental to the effectiveness of conventional chemotherapy and radiotherapy. The opposing strategy of targeting very high NO levels to tumours looks more promising in that it can be used to enhance conventional therapies as well as directly causing cell death. The available data provide convincing evidence that manipulation of endogenous NO using iNOS gene therapy can provide the basis for future clinical trials. The primary concern is that if iNOS expression is not tightly regulated at the target site, systemic hypotension can occur [121]. Improvement of vectors and delivery systems coupled with the study of appropriate NOS isoforms in large animal models are needed prior to translation to clinical use. Furthermore, NOS enzyme activity requires a panel of substrates and co-factors for full activity, and these may be missing from the target cell type. Therefore, another potential strategy is to use a cell-based approach, which will eliminate many of the toxicity concerns with the potential for considerable patient benefit. Cell-based approaches utilise the delivery of recombinant cells (rather than genes) to the target site, with the advantage that the expression of the gene of interest can be optimised prior to delivery. In order to make the NO-generating cells suitable for therapeutic delivery, Xu and colleagues [122] encapsulated these cells within a semipermeable alginate-poly-l-lysine membrane. This approach has been successful in animal models but to develop it for clinical use further work needs to be undertaken to improve delivery systems to minimise detrimental side effects and enhance positive treatment outcomes.
Conclusion
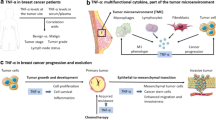
The precise role of NO in tumour pathophysiology has been the focus of numerous studies with involvement in a multitude of inter- and intra-cellular signalling pathways that are crucial to the malignant character of cancer. It is not surprising then that in heterogeneous tumours, a variety of responses have been observed following modification of NO levels. Thus, as has been referred before, the biological activity of NO depends on the source of NO generation, local concentration, tumour microenvironment, spatial and temporal constraints that can direct the function of NO. As shown in Fig. 4, the effects of NO at modest concentrations could be characterised as pro-malignant. At very high concentrations, however, NO acts as a potent anti-cancer agent, promoting apoptosis and inhibiting angiogenesis.
Mechanisms of action of NO on tumour cells. NO can induce tumour development or progression depending upon its local concentration and spatial and temporal distribution. Cellular responsiveness to NO might be an important determinant in the overall tumour response to NO, and its fundamental biology must be taken into account while interpreting experimental findings and for tailoring NO-based anti-cancer therapy
Abbreviations
- NO:
-
Nitric oxide
- NOS:
-
Nitric oxide synthase
- TNF-α:
-
Tumour necrosis factor-α
- IFN-γ:
-
Interferon-γ
- NF-κB:
-
Nuclear factor-κB
- HIF-1:
-
Hypoxia inducible factor-1
- HMGB1:
-
High-mobility group box 1
- MAPK:
-
Mitogen-activated protein kinase
- JNK:
-
c-Jun N-terminal kinase
- VEGF:
-
Vascular endothelial growth factor
References
Knowles RG, Moncada S (1994) Nitric oxide synthases in mammals. Biochem J 298:249–258
Nathan C, Xie QW (1994) Regulation of biosynthesis of nitric oxide. J Biol Chem 269:13725–13728
Elfering SL, Sarkela TM, Giulivi C (2002) Biochemistry of mitochondrial nitric-oxide synthase. J Biol Chem 277:38079–38086
Schmidt HH, Walter U (1994) NO at work. Cell 78:919–925
Hibbs JBJ (1991) Synthesis of nitric oxide from l-arginine: a recently discovered pathway induced by cytokines with antitumour and antimicrobial activity. Res Immunol 142:565–569
Kamijo R, Harada H, Matsuyama T, Bosland M, Gerecitano J, Shapiro D, Le J, Koh SI, Kimura T, Green SJ (1994) Requirement for transcription factor IRF-1 in NO synthase induction in macrophages. Science 263:1612–1615
Tendler DS, Bao C, Wang T, Huang EL, Ratovitski EA, Pardoll DA, Lowenstein CJ (2001) Intersection of interferon and hypoxia signal transduction pathways in nitric oxide-induced tumor apoptosis. Cancer Res 61:3682–3688
Melillo G, Musso T, Sica A, Taylor LS, Cox GW, Varesio LA (1995) Hypoxia responsive element mediates a novel pathway of activation of the inducible nitric oxide synthase promoter. J Exp Med 182:1683–1693
Kepp O, Tesniere A, Zitvogel L, Kroemer G (2008) The immunogenicity of tumor cell death. Curr Op Oncol 21:71–76
Sims GP, Rowe DC, Rietdijk ST, Herbst R, Coyle AJ (2010) HMGB1 and RAGE in Inflammation and Cancer. Annu Rev Immunol 28:367–388
Taguchi A, Blood DC, del Toro G et al (2000) Blockade of RAGE-amphoterin signalling suppresses tumour growth and metastases. Nature 405:354–360
Huttunen HJ, Kuja-Panula J, Sorci G et al (2000) Coregulation of neurite outgrowth and cell survival by amphoterin and S100 proteins through receptor for advanced glycation end products (RAGE) activation. J Biol Chem 275:40096–40105
Kuniyasu H, Chihara Y, Kondo H (2003) Differential effects between amphoterin and advanced glycation end products on colon cancer cells. Int J Cancer 104:722–777
Thomsen LL, Miles DW, Happerfield L, Bobrow LG, Knowles RG, Moncada S (1995) Nitric oxide synthase activity in human breast cancer. Br J Cancer 72:41–44
Cobbs CS, Brenman JE, Aldape KD, Bredt DS, Israel MA (1995) Expression of nitric oxide synthase in human central nervous system tumors. Cancer Res 55:727–730
Masri FA, Comhair SA, Koeck T, Xu W, Janocha A, Ghosh S, Dweik RA, Golish J, Kinter M, Stuehr DJ, Erzurum SC, Aulak KS (2005) Abnormalities in nitric oxide and its derivatives in lung cancer. Am J Respir Crit Care Med 172:597–605
Klotz T, Bloch W, Volberg C, Engelmann U, Addicks K (1998) Selective expression of inducible nitric oxide synthase in human prostate carcinoma. Cancer 82:1897–1903
Lagares-Garcia JA, Moore RA, Collier B, Heggere M, Diaz F, Qian F (2001) Nitric oxide synthase as a marker in colorectal carcinoma. Am Surg 67:709–713
Hajri A, Metzger E, Vallat F, Coffy S, Flatter E, Evrard S, Marescaux J, Aprahamian M (1998) Role of nitric oxide in pancreatic tumour growth: in vivo and in vitro studies. Br J Cancer 78:841–849
Weninger W, Rendl M, Pammer J, Mildner M, Tschugguel W, Schneeberger C, Stürzl M, Tschachler E (1998) Nitric oxide synthases in Kaposi’s sarcoma are expressed predominantly by vessels and tissue macrophages. Lab Invest 78:949–955
Ekmekcioglu S, Ellerhorst J, Smid CM, Prieto VG, Munsell M, Buzaid AC, Grimm EA (2000) Inducible nitric oxide synthase and nitrotyrosine in human metastatic melanoma tumors correlate with poor survival. Clin Cancer Res 6:4768–4775
Thomsen LL, Lawton FG, Knowles RG, Beesley JE, Riveros-Moreno V, Moncada S (1994) Nitric oxide synthase activity in human gynecological cancer. Cancer Res 54:1352–1354
Tschugguel W, Pustelnik T, Lass H, Mildner M, Weninger W, Schneeberger C, Jansen B, Tschachler E, Waldhör T, Huber JC, Pehamberger H (1999) Inducible nitric oxide synthase (iNOS) expression may predict distant metastasis in human melanoma. Br J Cancer 79:1609–1612
Loibl S, von Minckwitz G, Weber S, Sinn HP, Schini-Kerth VB, Lobysheva I, Nepveu F, Wolf G, Strebhart K, Kufmann M (2002) Expression of endothelial and inducible nitric oxide synthase in benign and malignant lesions of the breast and measurement of nitric oxide using electron paramagnetic resonance spectroscopy. Cancer 95:1191–1198
Dudzinski DM, Michel T (2007) Life history of eNOS: partners and pathways. Cardiovascular Res 75:247–260
Vakkala M, Paakko P, Soini Y (2000) eNOS expression is associated with the estrogen and progesterone receptor status in invasive breast carcinoma. Int J Oncol 17:667–671
Zheng PP, Hop WC, Luider TM et al (2007) Increased levels of circulating endothelial progenitor cells and circulating endothelial nitric oxide synthase in patients with gliomas. Ann Neurol 62:40–48
Lim KH, Ancrile BB, Kashatus DF et al (2008) Tumour maintenance is mediated by eNOS. Nature 452:646–649
Gosink EC, Forsberg EJ (1993) Effects of ATP and bradykinin on endothelial cell Ca2+ homeostasis and formation of cGMP and prostacyclin. Am J Physiol Cell Physiol 265:C1620–C1629
Ayajiki K, Kindermann M, Hecker M, Fleming I, Busse R (1996) Intracellular pH and tyrosine phosphorylation but not calcium determine shear stress-induced nitric oxide production in native endothelial cells. Circ Res 78:750–758
Wang L, Shi GG, Yao JC et al (2005) Expression of endothelial nitric oxide synthase correlates with the angiogenic phenotype of and predicts poor prognosis in human gastric cancer. Gastric Cancer 8:18–28
Ariel I, Hochberg A, Shochina M (1998) Endothelial nitric oxide synthase immunoreactivity in early gestation and in trophoblastic disease. J Clin Pathol 51:427–431
Bauer PM, Fulton D, Boo YC, Sorescu GP, Kemp BE, Jo H et al (2003) Compensatory phosphorylation and protein–protein interactions revealed by loss of function and gain of function mutants of multiple serine phosphorylation sites in endothelial nitric oxide synthase. J Biol Chem 278:14841–14849
Dudzinski DM, Igarashi J, Greif D, Michel T (2006) The regulation and pharmacology of endothelial nitric oxide synthase. Annu Rev Pharmacol Toxicol 46:235–276
Michell BJ, Chen ZZ, Tiganis T, Stapleton D, Katsis F et al (2001) Coordinated control of endothelial nitric-oxide synthase phosphorylation by protein kinase C and the cAMP-dependent protein kinase. J Biol Chem 276:17625–17628
Duda DG, Fukumura D, Jain RK (2004) Role of eNOS in neovascularization: NO for endothelial progenitor cells. Trends Mol Med 10:143–145
Chinje E, Stratford IJ (1997) The role of nitric oxide in growth of solid tumours: a balancing act. Essays Biochem 32:61–72
Lincoln TM, Dey N, Sellak HH (2001) cGMP-dependent protein kinase signaling mechanisms in smooth muscle: from the regulation of tone to gene expression. J Appl Physiol 91:1421–1430
Brunori M, Giuffre A, Forte E, Mastronicola D, Barone MC, Sarti P (2004) Control of cytochrome c oxidase activity by nitric oxide. Biochim Biophys Acta 1655:365–371
Thomas DD, Liu X, Kantrow SP, Lancaster JR Jr (2001) The biological lifetime of nitric oxide: implications for the perivascular dynamics of NO and O2. Proc Natl Acad Sci (USA) 98:355–360
Cooper CE, Giulivi C (2007) Nitric oxide regulation of mitochondrial oxygen consumption II: molecular mechanism and tissue physiology. Am J Physiol Cell Physiol 292:C1993–C2003
Stuehr DJ, Santolini J, Wang ZQ, Wei CC, Adak S (2004) Update on mechanism and catalytic regulation in the NO synthases. J Biol Chem 279:36167–36170
Ridnour LA, Thomas DD, Donzelli S, Espey MG, Roberts DD, Wink DA, Isenberg JS (2006) The biphasic nature of nitric oxide responses in tumor biology. Antioxid Red Signal 8:1329–1337
Leon L, Jeannin J-F, Bettaieb A (2008) Post-translational modifications induced by nitric oxide (NO): implication in cancer cells apoptosis. Nitric Oxide 19:77–83
Park HS, Yu JW, Cho JH, Kim MS, Huh SH, Ryoo K, Choi EJ (2004) Inhibition of apoptosis signal-regulating kinase 1 by nitric oxide through a thiol redox mechanism. J Biol Chem 279:7584–7590
Sumbayev VV (2003) S-nitrosylation of thioredoxin mediates activation of apoptosis signal-regulating kinase 1. Arch Biochem Biophys 415:133–136
DelaTorre A, Schroeder RA, Kuo PC (1997) Alteration of NF-kappa B p50 DNA binding kinetics by S-nitrosylation. Biochem Biophy Res Comm 238:703–706
Gopalakrishna R, Chen ZH, Gundimeda U (1993) Nitric oxide and nitric oxide generating agents induce a reversible inactivation of protein kinase C activity and phorbol ester binding. J Biol Chem 268:27180–27185
Park HS, Huh SH, Kim MS, Lee SH, Choi EJ (2000) Nitric oxide negatively regulates c-Jun N-terminal kinase/stress-activated protein kinase by means of S-nitrosylation. Proc Natl Acad Sci 97:14382–14387
Teng KK, Esposito DK, Schwartz GD, Lander HM, Hempstead BL (1999) Activation of c-Ha-Ras by nitric oxide modulates survival responsiveness in neuronal PC12 cells. J Biol Chem 274:37315–37320
Xu L, Eu JP, Meissner G, Stamler JS (1998) Activation of the cardiac calcium release channel (ryanodine receptor) by poly-S-nitrosylation. Science 279:234–237
MacMillan-Crow LA, Greendorfer JS, Vickers SM, Thompson JA (2000) Tyrosine nitration of c-SRC tyrosine kinase in human pancreatic ductal adenocarcinoma. Arch Biochem Biophys 377:350–356
West MB, Hill BG, Xuan YT, Bhatnagar A (2006) Protein glutathiolation by nitric oxide: an intracellular mechanism regulating redox protein modification. FASEB J 20:1715–1717
Maulik D, Ashraf QM, Mishra OP, Delivoria-Papadopoulos M (2008) Activation of p38 mitogen-activated protein kinase (p38 MAPK), extracellular signal-regulated kinase (ERK) and c-jun N-terminal kinase (JNK) during hypoxia in cerebral cortical nuclei of guinea pig fetus at term: role of nitric oxide. Neurosci Lett 439:94–99
Lander HM, Ogiste JS, Pearce SF, Levi R, Novogrodsky A (1995) Nitric oxide stimulated guanine nucleotide exchange on p21ras. J Biol Chem 270:7017–7020
Duhé RJ, Evans GA, Erwin RA, Kirken RA, Cox GW, Farrar WL (1998) Nitric oxide and thiol redox regulation of Janus kinase activity. Proc Natl Acad Sci 95:126–131
Tejedo JR, Cahuana GM, Ramirez R, Esbert M, Jiménez J, Sobrino F, Bedoya FJ (2004) Nitric oxide triggers the phosphatidylinositol 3-kinase/Akt survival pathway in insulin-producing RINm5F cells by arousing Src to activate insulin receptor substrate-1. Endocrinology 145:2319–2327
Lander HM, Jacovina AT, Davis RJ, Tauras JM (1996) Differential activation of mitogen-activated protein kinases by nitric oxide-related species. J Biol Chem 271:19705–19709
Lala PK, Chakraborty C (2001) Role of nitric oxide in carcinogenesis and tumour progression. Lancet Oncol 2:149–156
Pervin S, Singh R, Chaudhuri G (2008) Nitric Oide, Nω-hydroxy-l-arginine and breast cancer. Nitric Oxide 19:103–106
Thomas DD, Espey MG, Ridnour LA, Hofseth LJ, Mancardi D, Harris CC, Wink DA (2004) Hypoxic inducible factor 1alpha, extracellular signal-regulated kinase, and p53 are regulated by distinct threshold concentrations of nitric oxide. Proc Natl Acad Sci 101:8894–8899
Pervin S, Singh R, Hernandez E, Wu G, Chaudhuri G (2007) Nitric oxide in physiologic concentrations targets the translational machinery to increase the proliferation of human breast cancer cells: involvement of mammalian target of rapamycin/eIF4E pathway. Cancer Res 67:289–299
Schonhoff CM, Gaston B, Mannick JB (2003) Nitrosylation of cytochrome c during apoptosis. J Biol Chem 278:18265–18270
Millet A, Bettaieb A, Renaud F, Prevotat L, Hammann A, Solary E, Mignotte B, Jeannin JF (2002) Influence of the nitric oxide donor glyceryl trinitrate on apoptotic pathways in human colon cancer cells. Gastroenterology 123:235–246
Mannick JB, Schonhoff C, Papeta N, Ghafourifar P, Szibor M, Fang K, Gaston B (2001) S-Nitrosylation of mitochondrial caspases. J Cell Biol 154:1111–1116
Iyer AKV, Azad N, Wang L, Rojanasakul Y (2008) Role of S-nitrosylation in apoptosis resistance and angiogenesis. Nitric Oxide 19:146–151
Cook T, Wang Z, Alber S, Liu K, Watkins SC, Vodovotz Y, Billiar TR, Blumberg D (2004) Nitric oxide and ionizing radiation synergistically promote apoptosis and growth inhibition of cancer by activating p53. Cancer Res 64:8015–8021
Zhang Y, Xiong Y (2001) A p53 amino-terminal nuclear export signal inhibited by DNA damage-induced phosphorylation. Science 292:1910–1915
Wang X, Zalcenstein A, Oren M (2003) Nitric oxide promotes p53 nuclear retention and sensitizes neuroblastoma cells to apoptosis by ionizing radiation. Cell Death Differ 10:468–476
Yakovlev VA, Bayden AS, Graves PR, Kellogg GE, Mikkelsen RB (2010) Nitration of the tumor suppressor protein p53 at tyrosine 327 promotes p53 oligomerization and activation. Biochemistry 49:5331–5339
Hofseth LJ, Saito S, Hussain SP, Espey MG, Miranda KM, Araki Y, Jhappan C, Higashimoto Y, He P, Linke SP, Quezado MM, Zurer I, Rotter V, Wink DA, Appella E, Harris CC (2003) Nitric oxide-induced cellular stress and p53 activation in chronic inflammation. Proc Natl Acad Sci 1000:143–148
Cobbs CS, Samanta M, Harkins LE, Gillespie GY, Merrick BA, MacMillan-Crow LA (2001) Evidence for peroxynitrite-mediated modifications to p53 in human gliomas: possible functional consequences. Arch Biochem Biophys 394:167–172
Xu W, Liu L, Smith GC, Charles IG (2000) Nitric oxide upregulates expression of DNA-PKcs to protect cells from DNA-damaging anti-tumour agents. Nat Cell Biol 2:339–345
Jones MK, Tsugawa K, Tarnawski AS, Baatar D (2004) Dual actions of nitric oxide on angiogenesis: possible roles of PKC, ERK, and AP-1. Biochem Biophys Res Comm 318:520–528
Pervin S, Singh R, Freije WA, Chaudhuri G (2003) MKP-1-induced dephosphorylation of extracellular signal-regulated kinase is essential for triggering nitric oxide-induced apoptosis in human breast cancer cell lines: implications in breast cancer. Cancer Res 63:8853–8860
Chao JI, Kuo PC, Hsu TS (2004) Down-regulation of survivin in nitric oxide-induced cell growth inhibition and apoptosis of the human lung carcinoma cells. J Biol Chem 279:20267–20276
Garbán HJ, Bonavida B (2001) Nitric oxide inhibits the transcription repressor Yin-Yang 1 binding activity at the silencer region of the Fas promoter: a pivotal role for nitric oxide in the up-regulation of Fas gene expression in human tumor cells. J Immunol 167:75–81
Garbán HJ, Bonavida B (2001) Nitric oxide disrupts H2O2-dependent activation of nuclear factor kappa B. role in sensitization of human tumor cells to tumor necrosis factor-alpha-induced cytotoxicity. J Biol Chem 276:8918–8923
Tozer GM, Prise VE, Chaplin DJ (1997) Inhibition of nitric oxide synthase induces a selective reduction in tumor blood flow that is reversible with l-arginine. Cancer Res 57:948–955
Ishii Y, Ogura T, Tatemichi M, Fujisawa H, Otsuka F, Esumi H (2003) Induction of matrix metalloproteinase gene transcription by nitric oxide and mechanisms of MMP-1 gene induction in human melanoma cell lines. Int J Cancer 103:161–168
Wu J, Akaike T, Hayashida K, Okamoto T, Okuyama A, Maeda H (2001) Enhanced vascular permeability in solid tumor involving peroxynitrite and matrix metalloproteinases. Jpn J Cancer Res 92:439–451
Aurello P, Rossi Del Monte S, D’Angelo F, Cicchini C, Ciardi A, Bellagamba R, Ravaioli M, Ramacciato G (2009) Vascular endothelial growth factor C and microvessel density in gastric carcinoma: correlation with clinicopathological factors. Our experience and review of the literature. Oncol Res 17:405–411
Nakamura Y, Yasuoka H, Tsujimoto M, Yang Q, Tsukiyama A, Imabun S, Nakahara M, Nakao K, Nakamura M, Mori I, Kakudo K (2003) Clinicopathological significance of vascular endothelial growth factor-C in breast carcinoma with long-term follow-up. Mod Pathol 16:309–314
Ichinoe M, Mikami T, Shiraishi H, Okayasu I (2004) High microvascular density is correlated with high VEGF, iNOS and COX-2 expression in penetrating growth-type early gastric carcinomas. Histopathology 45:612–618
Giantonio BJ, Catalano PJ, Meropol NJ, O’Dwyer PJ, Mitchell EP, Alberts SR, Schwartz MA, Benson AB III (2007) Bevacizumab in combination with oxaliplatin, fluorouracil, and leucovorin (FOLFOX4) for previously treated metastatic colorectal cancer: results from the eastern cooperative oncology group study E3200. J Clin Oncol 25:1539–1544
Cahlin C, Gelin J, Delbro D, Lönnroth C, Doi C, Lundholm K (2000) Effect of cyclooxygenase and nitric oxide synthase inhibitors on tumor growth in mouse tumor models with and without cancer cachexia related to prostanoids. Cancer Res 60:1742–1749
Radomski MW, Jenkins DC, Holms L, Moncada S (1991) Human colorectal adenocarcinoma cells: differential nitric oxide synthesis determines their ability to aggregate platelets. Cancer Res 51:6073–6078
Dong Z, Staroselsky AH, Qi X, Xie K, Fidler IJ (1994) Inverse correlation between expression of inducible nitric oxide synthase activity and production of metastasis in K-1735 murine melanoma cells. Cancer Res 54:789–793
Xie K, Huang S, Dong Z, Juang SH, Gutman M, Xie QW, Nathan C, Fidler IJ (1995) Transfection with the inducible nitric oxide synthase gene suppresses tumorigenicity and abrogates metastasis by K-1735 murine melanoma cells. J Exp Med 181:1333–1343
Le X, Wei D, Huang S, Lancaster JR Jr, Xie K (2005) Nitric oxide synthase II suppresses the growth and metastasis of human cancer regardless of its upregulation of protumor factors. Proc Natl Acad Sci 102:8758–8763
Kiziltepe T, Hideshima T, Ishitsuka K, Ocio EM, Raje N, Catley L, Li C-Q, Trudel LJ, Yasui H, Vallet S, Kutok JL, Chauhan D, Mitsiades CS, Saavedra JE, Wogan GN, Keefer LK, Shami PJ, Anderson KC (2007) JS-K, a GST-activated nitric oxide generator, induces DNA double-strand breaks, activates DNA damage response pathways, and induces apoptosis in vitro and in vivo in human multiple myeloma cells. Blood 110:709–718
Postovit LM, Adams MA, Lash GE, Heaton JP, Graham CH (2004) Nitric oxide-mediated regulation of hypoxia-induced B16F10 melanoma metastasis. Int J Cancer 108:47–53
Konovalova NP, Goncharova SA, Volkova LM, Rajewskaya TA, Eremenko LT, Korolev AM (2003) Nitric oxide donor increases the efficiency of cytostatic therapy and reatrds the development of drug resistance. Nitric Oxide 8:59–64
Riganti C, Miraglia E, Viarisio D, Costamagna C, Pescarmona G, Ghigo D, Bosia A (2005) Nitric oxide reverts the resistance to doxorubicin in human colon cancer cells by inhibiting the drug efflux. Cancer Res 65:516–525
Muir CP, Adams MA, Graham CH (2006) Nitric oxide attenuates resistance to doxorubicin in three-dimensional aggregates of human breast carcinoma cells. Breast Cancer Res Treat 96:169–176
Cook JA, Krishna MC, Pacelli R, DeGraff W, Liebmann J, Mitchell JB, Russo A, Wink DA (1997) Nitric oxide enhancement of melphalan-induced cytotoxicity. Br J Cancer 76:325–334
Adams DJ, Levesque MC, Weinberg JB, Smith KL, Flowers JL, Moore J, Colvin OM, Silber R (2001) Nitric oxide enhancement of fludarabine cytotoxicity for BCLL lymphocytes. Leukemia 15:1852–1859
Yasuda H, Yamaya M, Nakayama K, Sasaki T, Ebihara S, Kanda A, Asada M, Inoue D, Suzuki T, Okazaki T, Takahashi H, Yoshida M, Kaneta T, Ishizawa K, Yamanda S, Tomita N, Yamasaki M, Kikuchi A, Kubo H, Sasaki H (2006) Randomized phase II trial comparing nitroglycerin plus vinorelbine and cisplatin with vinorelbine and cisplatin alone in previously untreated stage IIIB/IV non-small-cell lung cancer. J Clin Oncol 24:688–694
Huang LE, Bindra RS, Glazer PM, Harris AL (2007) Hypoxia-induced genetic instability-a calculated mechanism underlying tumor progression. J Mol Med 85:139–148
Brown JM (1999) The hypoxic cell: a target for selective cancer therapy-eighteenth Bruce F. Cain Memorial Award lecture. Cancer Res 59:5863–5870
Sandau KB, Fandrey J, Brune B (2001) Accumulation of HIF-1alpha under the influence of nitric oxide. Blood 97:1009–1015
Metzen E, Zhou J, Jelkmann W, Fandrey J, Brune B (2003) Nitric oxide impairs normoxic degradation of HIF-1α by inhibition of prolyl hydroxylases. Mol Biol Cell 14:3470–3481
Mateo J, Garcia-Lecea M, Cadenas S, Hernandez C, Moncada S (2003) Regulation of hypoxia-inducible factor-1alpha by nitric oxide through mitochondria-dependent and -independent pathways. Biochem J 376:537–544
Brown JM, Wilson WR (2004) Exploiting tumour hypoxia in cancer treatment. Nat Rev Cancer 4:437–447
McKeown SR, Cowen RL, Williams KJ (2007) Bioreductive drugs: from concept to clinic. Clin Oncol 19:427–442
Peters KB, Brown JM (1993) Tirapazamine: a hypoxia-activated topoisomerase II poison. Cancer Res 62:5248–5253
Chinje EC, Cowen RL, Feng J, Sharma SP, Wind NS, Harris AL, Stratford IJ (2003) Non-nuclear localized human NOSII enhances the bioactivation and toxicity of tirapazamine (SR4233) in vitro. Mol Pharmacol 63:1248–1255
Patterson LH (1993) Rationale for the use of aliphatic N-oxides of cytotoxic anthraquinones as prodrug DNA binding agents: a new class of bioreductive agent. Cancer Metastasis Rev 12:119–134
Cowen RL, Singh S, Chinje EC, Al-Assah R, Harris P, Dunk C, Stratford IJ (2005) Adenoviral delivery of inducible nitric oxide synthase (NOSII) enhances AQ4 N/radiation cytotoxicity within hypoxic tumor cells. AACR Meeting Abstracts 314-A
Robson T, Worthington J, McKeown SR, Hirst DG (2005) Radiogenic therapy: novel approaches for enhancing tumor radiosensitivity. Technol Cancer Res Treat 4:343–361
Gray LH, Green FO, Hawes CA (1958) Effect of nitric oxide on the radiosensitivity of tumour cells. Nature 182:952–953
Mitchell JB, Wink DA, DeGraff W, Gamson J, Keefer LK, Krishna MC (1993) Hypoxic mammalian cell radiosensitization by nitric oxide. Cancer Res 53:5845–5848
Verovski VN, Van den Berge DL, Soete GA, Bols BL, Storme GA (1996) Intrinsic radiosensitivity of human pancreatic tumour cells and the radiosensitising potency of the nitric oxide donor sodium nitroprusside. Br J Cancer 74:1734–1742
Wardman P, Rothkamm K, Folkes LK, Woodcock M, Johnston PJ (2007) Radiosensitization by nitric oxide at low radiation doses. Radiat Res 167:475–484
Singh S, Cowen RL, Chinje EC, Stratford IJ (2009) The impact of intracellular generation of nitric oxide on the radiation response of human tumor cells. Radiat Res 171:572–580
Li F, Sonveaux P, Rabbani ZN, Liu S, Yan B, Huang Q, Vujaskovic Z, Dewhirst MW, Li CY (2007) Regulation of HIF-1alpha stability through S-nitrosylation. Mol Cell 26:63–74
Abrams J (1992) Mechanisms of action of the organic nitrates in the treatment of myocardial ischemia. Am J Cardiol 70:30B–42B
Soler MN, Bobe P, Benihoud K, Lemaire G, Roos BA, Lausson S (2000) Gene therapy of rat medullary thyroid cancer by naked nitric oxide synthase II DNA injection. J Gene Med 2:344–352
Wang Z, Cook T, Alber S, Liu K, Kovesdi I, Watkins SK, Vodovotz Y, Billiar TR, Blumberg D (2004) Adenoviral gene transfer of the human inducible nitric oxide synthase gene enhances the radiation response of human colorectal cancer associated with alterations in tumor vascularity. Cancer Res 64:1386–1395
Worthington J, McCarthy HO, Barrett E, Adams C, Robson T, Hirst DG (2004) Use of the radiation-inducible WAF1 promoter to drive iNOS gene therapy as a novel anti-cancer treatment. J Gene Med 6:673–680
Halliwill JR, Minson CT, Joyner MJ (2000) Effect of systemic nitric oxide synthase inhibition on postexercise hypotension in humans. J Appl Physiol 89:1830–1836
Xu W, Liu LZ, Loizidou M, Ahmed M, Charles IG (2002) The role of nitric oxide in cancer. Cell Res 12:311–320
Acknowledgments
The authors acknowledge the support received from the Department of Biotechnology at Sharda University. We apologise to researchers whose findings that form the basis for our current knowledge in this field could not be cited due to space limitations.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Singh, S., Gupta, A.K. Nitric oxide: role in tumour biology and iNOS/NO-based anticancer therapies. Cancer Chemother Pharmacol 67, 1211–1224 (2011). https://doi.org/10.1007/s00280-011-1654-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-011-1654-4